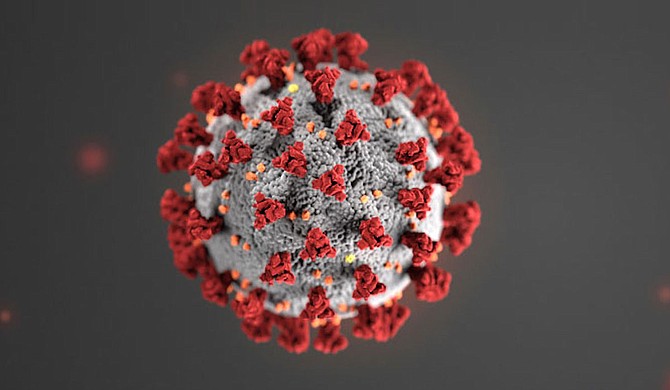
COVID-19 has arrived in Jackson. As the nation grapples with the extent of the crisis, the legislature and most business are shutting their doors. But there are vital steps individuals can take to protect themselves and their communities. Photo courtesy CDC.
"Please, if you're ill—if you have fever, please don't go to work. Stay home, and protect your coworkers," State Health Officer Dr. Thomas Dobbs pleaded from the open room in the core of the Mississippi Emergency Management Agency's Pearl headquarters. The March 16 press conference in the fortified recesses of the MEMA building, flanked by National Guardsmen, reflected the dire threat facing the state and the world at large.
Gov. Tate Reeves followed the presser with a video address of his own, delivered from isolation—Reeves had just returned the Friday before to the U.S. from a family trip to Spain, a country the virus hit hard.
"Our goal is over the next several days to stand up additional testing centers throughout Mississippi. And we're going to give the Department of Health as well as the Mississippi Emergency Management Agency access to Mississippi National Guard personnel to ensure the safety of our health care workers," Reeves said in the video address.
COVID-19 is here. And as the United States virtually shuts down amid fears of an overwhelmed health-care system and an unchecked pandemic, understanding the virus, its history, and how to mitigate its effects becomes an issue of national and local importance.
What is COVID-19?
COVID-19 is a "novel coronavirus," meaning a previously unidentified type of coronavirus, so named for the menacing spiked "crown" along its surface. Coronaviruses in general are a common affliction, and include the common cold. But COVID-19 is different, more comparable to the Spanish Influenza pandemic of just over a century ago, which infected half a billion people worldwide, killing between 50 million to 100 million of them.
Modern medicine will prevent the earth-shattering death toll of that pandemic, but we must not understate the virulence of COVID-19, its danger to everyone who acquires it, and our lack of preparedness for its arrival and spread.
COVID-19 Information Mississippians Need
Read breaking coverage of COVID-19 in Mississippi, plus safety tips, cancellations, more in the JFP's archive.
Is COVID-19 in Jackson?
Yes. The Mississippi Department of Health reported the first detected case of COVID-19 in Mississippi March 11, detected in a Forrest County man who recently traveled to Florida. He sought testing at a Hattiesburg clinic and is currently recovering in isolation at home, Dobbs said at a March 12 press conference.
MSDH announced the first cases of COVID-19 in Hinds County on March 15. Two students—one from Jackson State University and the other from the University of Mississippi Medical Center—are the capital city's first positive cases of the novel coronavirus.
The two Jackson residents who acquired the virus were also in quarantine at press time on March 17, but they clearly did not represent the only cases of the virus in the Jackson area. Recent research from Columbia University published in Science magazine estimates that "86% of all infections were undocumented," meaning that testing may reveal only a fraction of the virus' actual spread.
More distressingly, Dr. William Schaffner, professor at Vanderbilt University, told CNN on March 16 that "asymptomatic and mildly symptomatic transmission are a major factor in transmission for COVID-19," meaning individuals are capable of passing on the disease up to two weeks before displaying symptoms of their own infection.
In fact, by March 17, Hinds County had six confirmed cases.
Who does COVID-19 affect?
Experts say everyone is at risk of infection, serious illness, permanent respiratory damage and death from COVID-19. There has been much discussion of the category of people considered at "elevated risk" for acquiring and suffering a severe case of the virus, but its rapid spread in China and Italy in particular shows that COVID-19 is capable of maiming and killing the youngest and healthiest among us.
Still, we must not discard the group especially at risk from the virus. They include anyone over age 65, as well as anyone suffering from an immune system-compromising disease, including heart disease, lung disease, diabetes and more. Medical professionals worldwide have stressed that individuals with previously existing respiratory conditions are at particular risk of serious complications or death from COVID-19.
This does not mean the virus is a death sentence. Information sourced from China's Centers for Disease Control from the COVID-19 outbreak beginning in Wuhan revealed a 2.3% death rate across all age groups, a number Our World in Data noted is 12 to 24 times higher than the flu.
That death rate, broken down into age groups, reveals that around 18% of COVID-19 infections are fatal in individuals over age 80. Elsewhere, that number is proving to be higher. "Globally, about 3.4% of reported COVID-19 cases have died," World Health Organization Director General Tedros Adhanom Ghebreyesus said at a press briefing on March 3.
The Chinese Model
But numbers from the Chinese experience with the outbreak still weigh a majority of cases worldwide. And public-health experts like Dr. Bruce Aylward, senior adviser of the World Health Organization, assert that China was far more prepared for this virus than America is now because they acted quicker than the U.S. government to control the outbreak.
"They actually changed the course of a respiratory-borne outbreak without a vaccine, which was extraordinary," Aylward told NPR on March 8.
Early testing was important in China, even as the U.S. is woefully behind on having enough tests or other needed medical tools like ventilators. Donald G. McNeil, science and health reporter for The New York Times, explained the breadth of the Chinese model to MSNBC's Rachel Maddow on March 12. "(China's strategy was) Testing, testing, testing. Find the virus. ... If you go into any bus, train station, building, your temperature is taken."
China sent individuals displaying symptoms to specially designed fever clinics, created during the SARS outbreak and mothballed for just an occasion such as this pandemic, McNeil said.
At the clinics, the Chinese are heavily isolated, given a bacterial pneumonia test, a flu test, a CT scan and finally the COVID-19 test currently in such short supply in America. The entire process takes around four hours, with no exposure to the outside world, and critically, to their own families. "And that is the key element," McNeil said. "There is no home isolation. There is no home quarantine. (Because) 75% to 80% of the transmission in China was in family clusters."
The most recently updated total for COVID-19 cases in mainland China was 81,077, with 3,218 deaths, which WHO reported March 16. Notably, that is an increase from the last report of only 29 new cases. As China arrests the virus' spread, it continues to explode elsewhere, and so far nowhere more virulently than Italy.
The Italian Model
WHO's data on COVID-19's spread through Italy paint a stark, sobering picture for the rest of the world. Confirmed cases in Italy lingered around a hundred or so until late February. By the beginning of March, that number was over 1,000—then a week later, almost 6,000. WHO's most recent situation report at the time of this article's writing only places the total infections in the country at 24,747. That number will continue to rise, and the rapidity with which it spiked has plunged the country's medical system into chaos.
Shortages of ICU beds, ventilators and medical professionals alike have left the afflicted desperate for care and without the equipment necessary to receive it. On March 11, The Atlantic reported new guidelines for Italy's worsening crisis, a morbid form of triage more suited for trench warfare than municipal hospitals.
"Informed by the principle of maximizing benefits for the largest number," The Atlantic's translation of the document reads, "the allocation criteria need to guarantee that those patients with the highest chance of therapeutic success will retain access to intensive care." In plain English, this means some of the most vulnerable patients—the oldest and weakest victims of the virus—must simply be left to die.
This is precisely the reason for the nationwide shutdown, first in Northern Italy, at the outbreak's epicenter, then across the country and now here in the United States, which CDC data show to be on a horrifyingly similar trajectory to Italy's. The potential for a 2% death rate for COVID-19, itself a dizzying prospect that could leave millions dead in the worst case scenario, requires a functioning health-care system that is capable of actually serving all of the critically infected at once.
The newest data from Italy at the time of this article's writing showed 1,809 deaths for the country's 24,747 confirmed infections: a death rate of roughly 7.3%. These numbers almost certainly do not reflect the many mild cases that went undiagnosed or unexamined, but they still represent an ever-escalating nightmare.
Experts in the U.S. and abroad say any attempt to address COVID-19 without the mass testing of countries like China and South Korea could spiral into the Italian catastrophe. "What is very clear," Richard Neher, a biologist at the University of Basel told the news site Vox, is that "without a drastic reduction in transmission of the virus, health systems will be overwhelmed."
Mississippi Reacts
As of March 17, MSDH had run 389 COVID-19 tests in Mississippi, 21 of them returning positive results. Early on, it appeared that many of the cases were the result of outside transmission to Mississippi residents returning from out of state before coming down with the virus. This will not be the case for much longer. "There will be cases from individuals who did not travel outside of Mississippi. That will be the new norm," State Epidemiologist Dr. Paul Byers said at a March 13 press conference.
UMMC enacted a strict new visitation policy this week, limiting entrances and exits to the hospital complex and preventing visitation for most adult patients, mirroring the heightened security at UMMC facilities in other counties.
"This will test all of us like nothing we have experienced in many years," UMMC School of Medicine Dean LouAnn Woodward said in a March 15 email to faculty, staff and students. "I know you will join me in remaining calm and professional, and at all times serving our patients and each other with the very best we have to offer."
On March 12, Dobbs announced expanded access to the Public Health Lab's COVID-19 testing procedures. The testing services available at MSDH mean all primary-care providers in Mississippi may use courier services to send potential COVID-19 samples to the state's testing facility as well as private facilities capable of confirming or dispelling a potential infection.
Preparedness for COVID-19 sample collection and testing in the capital city came in fits and starts. As of early afternoon Friday, March 13, the Jackson Free Press had yet to successfully reach a single health-care provider in the Jackson metro capable of ordering a COVID-19 test. That was the same day that state health officials said they had been calling clinics all day to explain the procedure.
Some institutions referred the Jackson Free Press back to MSDH, still unaware that they had the capacity to collect samples for COVID-19. That afternoon, MSDH acknowledged it was still reaching out to clinics and physicians to instruct them in addressing the pandemic, making over 400 calls on March 13 alone.
By Monday, March 16, some of that confusion seemed to have abated. Clinics and hospitals the Jackson Free Press called Monday morning had a much better grasp of the process of COVID-19 sample retrieval and testing. Some, but not all clinics contacted, could confirm that they had the capacity to gather COVID-19 samples.
On Sunday, the Centers for Disease Control announced new guidelines advising against gatherings of 50 people or more, specifically targeted at "large events and mass gatherings (including) conferences, festivals, parades, concerts, sporting events, weddings, and other types of assemblies."
By Monday, President Donald Trump amended that number to 10 people: a much more stringent advisory that pressed many states to shutter bars and restaurants after weekend photos of crowded weekend revelry shocked a scared nation. At a press conference on March 16, however, Dobbs declined to recommend the closure of Mississippi's restaurants and bars.
That same day, Jackson Mayor Chokwe A. Lumumba declared a civil emergency in the City of Jackson, closing down non-essential government services and sending many state employees to work from home. Lumumba also urged businesses like restaurants to, at minimum, begin take-out and delivery only services to curtail large groups. "Do what is necessary to limit crowds and to ensure adequate spacing between patrons sitting down at your restaurant," Lumumba said at a March 16 press event. He did not discount taking more draconian steps, if warranted. "If need be, we will implement more extreme measures or more severe measures going forward," he said.
Those restrictions, as well as those of the CDC, do not apply to the Mississippi Legislature, both chambers of which gaveled in at 4 p.m. March 16. The week before, Lt. Gov. Delbert Hosemann announced new restrictions on legislative attendance, preventing access to the Capitol for most of the public, sending pages home and barring lobbyists from the Capitol rotunda.
"We intend to work as long as is humanly possible," Hosemann said at a Friday press conference in the Capitol press room. As of Monday morning, March 16, legislative sessions in 20 states across the U.S. had postponed or adjourned to avoid providing a vector for the virus to spread.
By mid-day on March 17, the Mississippi legislative session was on hold. The Legislature passed bills before adjourning that extend the session and provide state employees with pay during the quarantine period. But House Republicans killed a bill by Rep. Robert Johnson III, D-Natchez, that would have required the Mississippi Department of Employment Security to provide paid leave for employees of private businesses laid off or furloughed because of COVID-19.
Part of the initial hesitation to suspend the session, one source told this reporter, was a desire to pass emergency legislation to "ease the burden on citizens." Such legislation could pass quickly before the Legislature shuts down to weather the global pandemic's spread.
Sen. Chris McDaniel, R-Ellisville, acknowledged the threat the virus posed to public health and the unique danger of the disease spreading through the Legislature. "We each represent a different part of the state—If somebody were to be infected there it would certainly be possible for us to take it back to our districts," he said in a phone interview on March 16.
By Tuesday, March 17, plans to indefinitely suspend the legislature were underway, with House Speaker Philip Gunn telling the chamber that "We have decided to work to suspend the session."
Later, in a livestream press conference from the Capitol rotunda, Gunn and Hosemann joined to explain the session's suspension, planned for Wednesday, March 18. "The House is adjourned for this time period," Gunn said.
"This has not been going on in a vacuum," Hosemann said. "We have met with the state economist, and the Department of Revenue." Hosemann said regular Thursday meetings with state financial officials would help project the cost of the quarantine period.
Hosemann wrapped up the press conference with words of encouragement for Mississippians preparing for a long quarantine. After weathering this "most unusual" pandemic, Hosemann promised that "we will again join our friends and our neighbors at church, social gatherings, sporting events—at the things we normally do as a society to make our lives fulfilled. Our lives will return to normal. They're going to return to normal when we get through this. These challenges are temporary. But our persistence is permanent. And we will survive this."
Hosemann closed his remarks with characteristic optimism. "Hope to see y'all in two weeks," he said.
Read full, ongoing coverage of COVID-19 in Mississippi at jfp.ms/coronavirus. Email state reporter Nick Judin at [email protected]. Reporter Seyma Bayram and state intern Julian Mills contributed to this report.
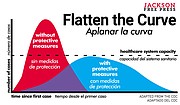
Flatten the Curve
Aplanar la Curva
The above graph illustrates why the entire nation is shutting down. COVID-19 is a dangerously virulent disease. What's worse, it is also transmissible for up to 14 days before symptoms begin to show. A new study in Science Magazine reports that up to 86% of COVID-19 cases go undetected. Severe cases of the disease require hospital beds and ventilators, both of which are in limited supply.
These facts, taken together, explain why social distancing, intense hygiene and limiting public gatherings may be our best defense against the worst-case scenario, the kind presently unfolding in Italy. If we take all measures to slow the spread of the virus through the population, hospitals will have the time and space needed to properly treat the afflicted. If we are not vigilant, however, and allow the virus to spread through large social gatherings and public spaces, the severely ill may overwhelm our hospitals' capacity.
There is no silver bullet for defeating COVID-19. Sham treatments, like self-diagnosis through a breathing test or snake oil "cures" hawked online, are useless. Only a series of professional medical tests can discern between COVID-19 and the common flu, and scientists developing a vaccine say it is still a year or more away. What you can do now to protect yourself and the most vulnerable members of your community is to follow CDC guidelines, limit contact with others and practice strong hygienic habits.
La grafica de arriba es la mejor ilustracion para explicar por que la nacion entera esta tomando medidas de contencion. El Covid-19 es una enfermedad peligrosa y contagiosa. Lo peor es que se puede transmitir hasta 14 dias antes de que los sintomas comiencen a aparecer.
Un nuevo estudio en Science Magazine indica que hasta 86% de los casos del Covid-19 pasan desapercibidos. Los casos mas graves de esta enfermedad requieren camas de hospital y ventiladores, cuya disponibilidad es limitada.
Estos hechos, en conjunto, explican por que practicar el distanciamiento social, mantener una rigurosa higiene, y evitar los lugares concurridos, pueden ser nuestra mejor estrategia contra el peor escenario posible, como el que actualmente se desarrolla en Italia.
Si tomamos todas las medidas para retrasar la propagacion del virus a traves de la poblacion, los hospitales tendran el tiempo y el espacio necesarios para atender a los afectados adecuadamente. Sin embargo, si no somos cuidadosos y dejamos que el virus se propague a traves de reuniones multitudinarias y espacios publicos, los pacientes mas delicados podrian superar la capacidad de nuestros hospitales.
No hay una cura magica para vencer al Covid-19. Los tratamientos improvisados, como el autodiagnostico con una prueba de respiracion, o los remedios milagrosos que se anuncian en internet son inutiles. Solo mediante una serie de examenes medicos es posible distinguir el Covid-19 de la gripe comun, y los cientificos que estan trabajando en el desarrollo de una vacuna dicen que esta tardara un ano o mas en estar lista.
Lo que puedes hacer en este momento para protegerte y proteger a los miembros mas vulnerables de tu comunidad es atender las recomendaciones de los CDC, reducir el contacto con otros, y seguir una higiene muy rigurosa.
Read the JFP’s coverage of COVID-19 at jacksonfreepress.com/covid19. Get more details on preventive measures here. Read about announced closings and delays in Mississippi here. Read MEMA’s advice for a COVID-19 preparedness kit here.
Email information about closings and other vital related logistical details to [email protected].
Email state reporter Nick Judin, who is covering COVID-19 in Mississippi, at [email protected] and follow him on Twitter at @nickjudin. Seyma Bayram is covering the outbreak inside the capital city and in the criminal-justice system. Email her at [email protected] and follow her on Twitter at @seymabayram0.
More stories by this author
- Vaccinations Underway As State Grapples With Logistics
- Mississippi Begins Vaccination of 75+ Population, Peaks With 3,255 New Cases of COVID-19
- Parole Reform, Pay Raises and COVID-19: 2021 Legislative Preview
- Last Week’s Record COVID-19 Admissions Challenging Mississippi Hospitals
- Lt. Gov. Hosemann Addresses Budget Cuts, Teacher Pay, and Patriotic Education





Comments
Use the comment form below to begin a discussion about this content.
comments powered by Disqus