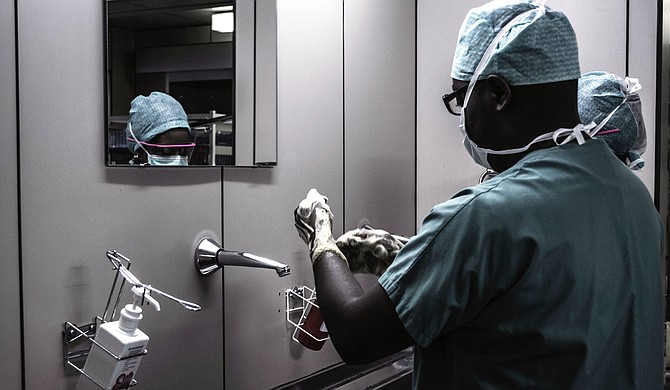
Research suggests Black patients have better outcomes when treated by Black doctors and nurses. Yet, only 5% of doctors nationwide are Black, and only 2% are Black women, according to the Association of American Medical Colleges. Photo by Piron Guillaume on Unsplash
JACKSON, Miss. (AP) — Dr. Janice Bacon was exactly the person Kay McField hoped to talk to when she found herself spending most of her days in bed, feeling too depressed to get up as the coronavirus pandemic threatened those around her.
As she watched those closest to her test positive for the virus — a goddaughter and her uncle, whom she cares for, among them — McField said she was terrified that she or her daughter, who both suffer from autoimmune diseases, would fall ill. When she wasn't in bed, the 51-year-old single mother was cleaning her house compulsively.
“It was just this constant panic," she said, her arms pressed to her chest. “I wanted to talk to someone I knew was going to listen, who I could trust.”
A Black primary care physician practicing in Mississippi for nearly four decades, Bacon works at an all-African American-run trio of community health centers in Hinds County, where the population is overwhelmingly Black — and where the most coronavirus cases have been reported in the state.
Most of the families that Bacon and the more than 50 other doctors, nurses and social workers serve are African American, low-income and living with health conditions like heart disease, diabetes and asthma that are more common among Black Americans. Even before the coronavirus, many were dealing with depression and anxiety, Bacon said.
During the pandemic, those problems have been exacerbated. Many clinic patients are essential workers expected to work in-person even as coronavirus cases have skyrocketed in Mississippi. While testing is free for community health center patients, delays are a major issue, Bacon said, with some families waiting up to two weeks for results.
Bacon said she has seen people scrape together $187 to pay for a rapid test at other clinics that don't accept Medicaid, in hopes of returning to work faster and not losing their jobs.
"There’s this feeling of, ’I just can’t handle it all,'” Bacon said. “We are seeing serious mental health consequences.”
Meanwhile, families are struggling to find child care and put food on the table. Two of the largest school districts in the area decided to start virtually, creating more barriers for families that don't have internet access, or if they do, don't know how to use devices for online learning or can't afford them.
Research suggests Black patients have better outcomes when treated by Black doctors and nurses. Yet, only 5% of doctors nationwide are Black, and only 2% are Black women, according to the Association of American Medical Colleges.
The Central Mississippi Health Services clinic where Bacon works is on the campus of Tougaloo College, a historically Black institution that was a gathering place for civil rights activists in the 1960s. As part of the national network of community health centers, it receives federal funding to serve communities designated as medically under-served areas, with fees adjusted based on ability to pay.
Over generations, Bacon has built trust in a community generally skeptical of the health care system and made her Black patients feel they have a safe place to go for medical care.
“It’s meaningful to be taken care of by someone who looks like you, who understands you,” McField said. “Other doctors go into the exam room, and they don’t ask your name. And me, when I go there and be treated that way, I’m not going back no more.”
Raised 90 miles from Jackson in Natchez, Mississippi, Bacon suffered from severe asthma. Her pediatrician would treat her at his house when she would have attacks, even in the middle of the night. That inspired her to become a community doctor.
In her office, Bacon has a portrait of Michelle and Barack Obama on the wall, and photos of her patients on a bulletin board. McField’s daughter Ella’s high school graduation photo is among them. Ella, who is starting college this fall, says she has wanted to be a doctor or a nurse since she was little because of Bacon.
Bacon has cared for McField's family for generations. She was the doctor for McField’s mother and her 10 siblings, and now she looks after their children. McField said her brother drove three hours from Memphis so his children could be seen by Bacon.
When she has gone elsewhere for medical care, McField said, she has been talked down to, misdiagnosed or dismissed by doctors. Bacon said there is still a lot of implicit bias in the health care system, and she has seen how it hurts her patients.
When McField opened up to Bacon about her depression during the pandemic, the doctor introduced her to a social worker who helped her find coping strategies — writing in a journal, taking a break from watching the news and praying. She said she's doing a lot better.
Clinic staff members say they see their role as more than treating their patients’ physical health. They work with food banks, churches and other social services to make sure people have access to food and clean drinking water while in isolation, as well as transportation when they can venture out again.
“They can get your high blood pressure medication refilled, and then come down the hallway and talk about why it was up 20 points this week,” said social worker Chinnika Crisler. “Maybe it’s because the unemployment stimulus just ended, and 'I really don’t know how to pay my rent next month, so now I’m not sleeping.”'
The pandemic has made running some of the center's normal programming challenging. Nutrition sessions for preteens and their parents at risk for obesity were halted in person. Respite care for parents of children with significant health conditions — something Bacon knows is desperately needed right now — has been on pause until providers find a safe way to visit patients' homes.
But there is still much to do. On one recent day, Crisler was helping a single mother of three apply for benefits through the Family and Medical Leave Act because she wasn't able to balance working and taking care of her three kids at home by herself.
Clinician and social worker Lisa Williams said that although the pandemic has made a lot of the problems that patients deal with worse, they aren't anything new.
“People have been struggling for a long, long time," she said.
Copyright Associated Press. All rights reserved. This material may not be published, broadcast, rewritten, or redistributed.


Comments
Use the comment form below to begin a discussion about this content.
comments powered by Disqus